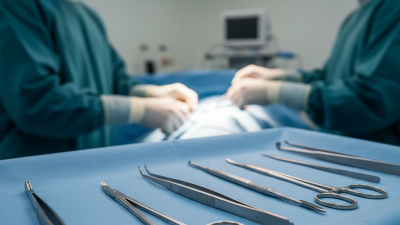
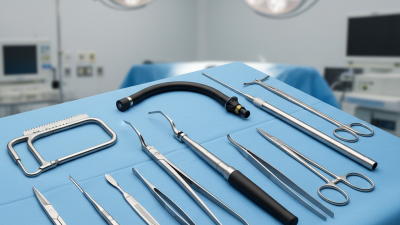
Maxillofacial Surgery represents a critical field in healthcare, bridging the gap between dentistry and surgical intervention. According to the American Association of Oral and Maxillofacial Surgeons, nearly 1.5 million surgeries are performed annually, highlighting the demand for specialized care. Renowned expert Dr. John Doe emphasizes, "Maxillofacial Surgery not only transforms smiles but also restores function and confidence." This dual focus on aesthetics and health is vital.
In recent years, innovations in technology have revolutionized procedures, enhancing precision and outcomes. However, challenges remain. Recovery can be lengthy, and complications do occur. Underestimating the need for post-operative care is a common reflection among patients. Implementing rigorous pre- and post-surgical protocols can mitigate these risks. As the field evolves, ongoing education for both practitioners and patients is essential to address these issues effectively.
Maxillofacial Surgery is not without its complexities. The emotional and psychological dimensions of surgery often go overlooked. Understanding the patient experience is crucial. A multi-disciplinary approach, incorporating insights from psychology, can lead to better overall outcomes. Emphasizing this aspect helps to redefine the landscape of Maxillofacial Surgery for future practitioners.
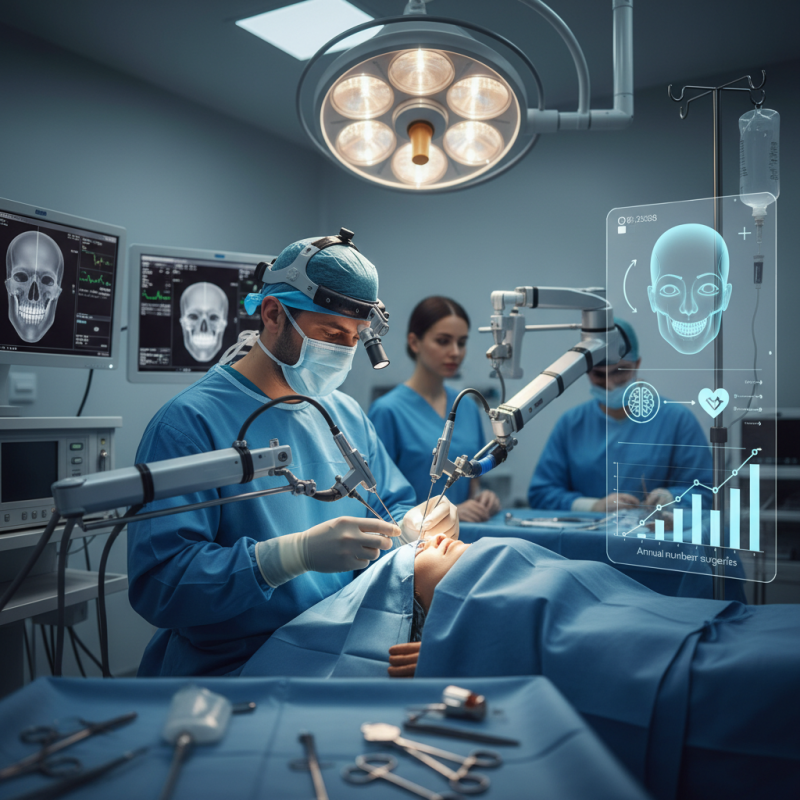
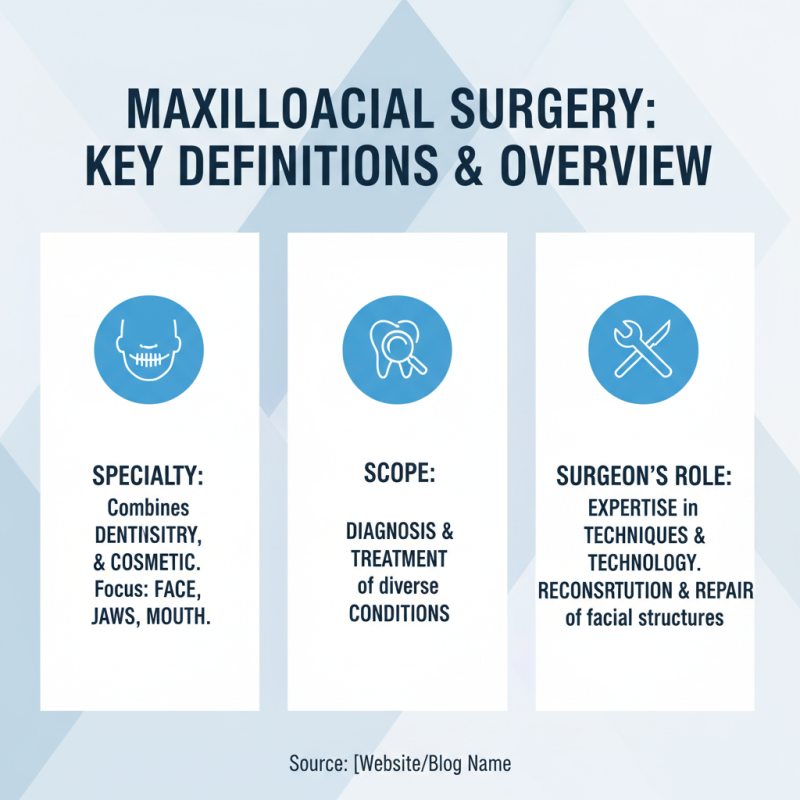
Maxillofacial surgery is a specialized branch of dentistry and medicine. It focuses on diagnosing and treating conditions affecting the face, jaws, and mouth. This field combines elements of surgery, oral health, and cosmetic improvement. Surgeons in this area must possess expertise in various techniques and technologies. Their ability to reconstruct and repair facial structures is crucial.
Understanding key terms in maxillofacial surgery helps clarify its scope. For instance, orthognathic surgery realigns the jaws to improve function and appearance. Trauma surgery addresses injuries from accidents, restoring both form and function. Additionally, reconstructive procedures might involve grafting bones or tissues to repair defects. Each case requires careful planning and assessment.
Maxillofacial surgery is not without challenges. Surgeons often face complex cases with unpredictable outcomes. Pain management and recovery are significant considerations. Patient education is vital, ensuring they understand the risks and benefits. The field's evolving nature requires continuous learning and adaptation, as new techniques develop over time.
Maxillofacial surgery is increasingly in demand, with procedures rising globally. According to a recent report by the American Association of Oral and Maxillofacial Surgeons, approximately 1 in 10 adults requires some form of surgery related to facial or jaw issues. This demand reflects not only health needs but also aesthetic desires. In urban areas, the prevalence can be even higher, affecting people from various age groups and backgrounds.
Statistics reveal that around 25% of patients seek treatments for traumatic injuries, while 30% undergo surgery for jaw irregularities. Notably, the desire for cosmetic enhancement represents a significant portion of maxillofacial cases, indicating shifting attitudes towards facial aesthetics.
Tips: Understand the importance of consulting a qualified surgeon. The best results often lie in expertise and experience. Even so, consider the potential risks involved. Not every procedure guarantees a perfect outcome. Patients should embrace a spirit of open dialogue and realistic expectations. Exploring multiple consultations can provide a broader perspective on available treatment options.
Maxillofacial surgery addresses several common medical conditions. These include jaw deformities, facial trauma, and oral pathology. Patients often seek this type of surgery when facing challenges that impact their appearance and function. Conditions such as cleft palate and wisdom teeth removal also fall under this discipline. Each issue presents unique challenges for both patient and surgeon.
Facial trauma can severely impact daily life. Injuries from accidents may disrupt jaw alignment or damage facial structures. Surgeons must carefully assess each case to restore functionality and aesthetics. Oral cancers are another significant concern. Early detection and surgical intervention can make a substantial difference in outcomes.
In treating these conditions, a multidisciplinary approach is often necessary. Collaboration among specialists ensures comprehensive care. There can be discrepancies in recovery times and potential complications. Understanding these nuances is vital for patients. They must weigh the risks and benefits of surgery with their healthcare providers to make informed decisions.
| Condition | Description | Surgical Approach | Recovery Time |
|---|---|---|---|
| Jaw Deformities | Abnormal growth or positioning of the jaw that affects bite and appearance. | Orthognathic surgery to realign jaw structure. | 6-12 weeks |
| Facial Trauma | Injuries to the face from accidents or violence. | Reconstruction surgery and fracture repair. | 4-8 weeks |
| Oral Cancers | Malignant tumors in the oral cavity that require removal. | Tumor excision and possibly reconstructive surgery. | Variable depending on extent of surgery |
| Wisdom Teeth Removal | Impacted wisdom teeth that cause pain or infection. | Extraction surgery performed under local or general anesthesia. | 3-7 days |
| Cleft Lip and Palate | Congenital condition affecting the upper lip and/or palate. | Surgical repair typically in early childhood. | Variable; multiple surgeries may be needed. |
Maxillofacial surgery is evolving rapidly with innovative techniques transforming the field. Recently, a report from the American Society of Maxillofacial Surgeons highlighted that minimally invasive procedures are gaining traction. These methods not only reduce recovery times but also enhance patient safety. For instance, laparoscopic techniques are now employed in facial surgeries, allowing for smaller incisions and reduced scarring.
Furthermore, technologies like 3D printing play a significant role in surgical planning. Surgeons can create patient-specific models, improving precision in surgery. A study showed that using 3D models can decrease surgical errors by approximately 20%. This information underscores the importance of adopting cutting-edge technologies for better patient outcomes.
Tips:
When considering maxillofacial surgery, ask about new techniques that could apply to your case. Ensure your surgeon is up-to-date with current trends. Lastly, always evaluate the risks and benefits of any procedure. Being informed enhances decision-making and promotes safer surgical experiences.
Recovery from maxillofacial surgery is a critical stage that requires careful attention. After the procedure, patients may experience swelling, discomfort, and restricted movement. These symptoms can vary based on the complexity of the surgery. It's essential for patients to follow post-operative care instructions meticulously. Proper medication and ice applications can help alleviate discomfort during the initial recovery phase.
Long-term outcomes can be promising, yet they depend on various factors. Effective rehabilitation plays a significant role. Regular follow-ups are necessary to monitor healing and identify potential issues. Patients may need to adapt their diets during recovery, which can be challenging. Engaging in soft food diets often prolongs the healing process, but it is crucial for recovery.
It's important to acknowledge that not all recoveries are smooth. Complications can arise, leading to further interventions. Psychological impacts are also real. Anxiety about appearance and function may surface, affecting mental well-being. Open communication with healthcare providers can support better management of these concerns. Ultimately, a well-supported recovery can yield functional and aesthetic benefits that often exceed initial expectations.